Fred Trotter
Malignant computation
To properly serve society, cryptocurrencies must support computer hardware that is useful for other things.
Cryptocurrencies, like bitcoin, could revolutionize money to the same degree that the Internet has revolutionized communication. However, like any economic marketplace, human exuberance is the greatest threat to the cryptocurrency phenomenon. Markets fail to the degree that the market can be dominated by those seeking personal gain, and markets succeed to the degree that they resist domination and focus on benefiting society at large.
The cryptocurrency market place is in danger of becoming so focused on profitability, that it loses sight of the potential computational benefits that it could provide to society. I hope that this article will influence designers of cryptocurrencies to attempt to avoid computational malignancy.
Many people regard the success or failure of the market to be the degree that it works for them, rather than for society as a whole. One of the fundamental motivations for cryptocurrency is the general sense that banks, governments and markets have failed to protect the interest of the common man. It is not an accident that the rise of bitcoin began shortly after the sub-prime mortgage crisis. Read more…
Doctors vs Data
There is a storm brewing in Healthcare. Doctors have been in charge of healthcare for a long time, and have become comfortable, sometimes even arrogant, with their authority and power. But dumb data beats smart doctors every time. Forward thinking doctors are embracing data, with surprising grace and humility. Others are having much more trouble adjusting.
Doctors, historically, have been the “end of the discussion” on clinical matters. Doctors make the diagnosis, they make the calls in the surgery suite, they get to decide if someone is suffering enough to justify pain medications, they frequently decide whether someone is mentally incompetent or merely eccentric. Our society places a lot of trust in doctors, because they have the training needed to make really hard choices.
Doctors, as a group, have been in charge of how healthcare operates for centuries. In times past, the only way to determine whether a doctor was doing a good job was to become a doctor yourself, and then perform case reviews. Even in court, if you wanted to refute a doctor, you needed another doctor.
Doctor Data made to order
Recently, Health and Human Services (HHS) Centers for Medicare and Medicaid Services (CMS) released a request for public comment on how they should handle the reversal of an injunction that prevented them from revealing specific information about how doctors perform.
The mere request by the federal government for feedback on how best to use their new capacity to leverage Big Data to improve the healthcare system is a breath of fresh air. It is a welcome change from Snowden/NSA news and is a welcome indication that somewhere in the Federal Government there exists someone who understands technology policy well enough to not have “Aim gun at own toes” on their todo list. So we should all enjoy that for a moment.
Bigger Data Leaner Pharma
Open source communities to help find the next blockbuster drug
Big drug companies are not what they used to be. It is harder to find new drug candidates, to test them, and to get them approved than ever before. Drugs that are “mere chemicals” are becoming more and more complex. Frequently, new drugs require DNA interaction, which requires them to be manufactured through a mostly automated cellular process rather than just mixing the right components in the right order. Just the changes to the refrigeration requirements for these new drugs represents a challenge to drug manufacturers, pharmacies and hospitals.
Combined, these difficulties create a combustible business environment that can ignited by the pressure of expiring patents. Experts estimate that the approval process ensures that a drug company actually gets only about 12 years of exclusivity before a 20-year patent wears off. So in pharma-land, the march of popular medications to generic status forces the original developers into the famous Innovators Dilemma. Most companies face competition from the generic versions of their own previous work.
Read more…
Moving to the open health-care graph
A network graph approach to modeling the health-care system.
To achieve the the triple aim in healthcare (better, cheaper, and safer), we are going to need intensive monitoring and measurement of specific doctors, hospitals, labs and countless other clinical professionals and clinical organizations. We need specific data and specific doctors.
In 1979 a Federal judge in Florida sided with the AMA to prevent these kinds of provider-specific data sets violated doctor privacy. Last Friday, a different Florida judge reversed the 1979 injunction, allowing provider identified data to be released from CMS under FOIA requests. Even without this tremendous victory for the Wall Street Journal, there was already a shift away from aggregation studies in healthcare towards using Big Data methods on specific doctors to improve healthcare. This critical shift will allow us to determine which doctors are doing the best job, and which are doing the worst. We can target struggling doctors to help improve care, and we can also target the best doctors, so that we can learn new best practices in healthcare.
Evidence-based medicine must be targeted to handle specific clinical contexts. The only really open questions to decide are “how much data should we relese” and “should this be done in secret or in the open.” I submit that the targeting should be done at the individual and team level, and that this must be an open process. We need to start tracking the performance and clinical decisions of specific doctors working with other specific doctors, in a way that allows for public scrutiny. We need to release uncomfortably personal data about specific physicians and evaluate that data in a fair manner, without sparking a witch-hunt. And whether you agree with this approach or not, it’s already underway. The overturning of this court case will only open the flood gates further. Read more…
How crowdfunding and the JOBS Act will shape open source companies
New regulations could mark the end of proprietary finance.
Currently, anyone can crowdfund products, projects, causes, and sometimes debt. Current U.S. Securities and Exchange Commission (SEC) regulations make crowdfunding companies (i.e. selling stocks rather than products on crowdfund platforms) illegal. The only way to sell stocks to the public at large under the current law is through the heavily regulated Initial Public Offering (IPO) process.
The JOBS Act will soon change these rules. This will mean that platforms like Kickstarter will be able to sell shares in companies, assuming those companies follow certain strict rules. This change in finance law will enable open source companies to access capital and dominate the technology industry. This is the dawn of crowdfunded finance, and with it comes the dawn of open source technology everywhere.
The JOBS Act is already law, and it required the SEC to create specific rules by specific deadlines. The SEC is working on the rulemaking, but it has made it clear that given the complexity of this new finance structure, meeting the deadlines is not achievable. No one is happy with the delay but the rules should be done in late 2013 or early 2014.
When those rules are addressed, thousands of open source companies will use this financial instrument to create new types of enterprise open source software, hardware, and bioware. These companies will be comfortably funded by their open source communities. Unlike traditional venture-capital-backed companies, these new companies will narrowly focus on getting the technology right and putting their communities first. Eventually, I think these companies will make most proprietary software companies obsolete. Read more…
Preferred structures for cleaned-up doctor data
Which data formats should the DocGraph project support?
The DocGraph project has an interesting issue that I think will become a common one as the open data movement continues. For those that have not been keeping up, DocGraph was announced at Strata RX, described carefully on this blog, and will be featured again at Strata 2013. For those that do not care to click links, DocGraph is a crowdfunded open data set, which merges open data sources on doctors and hospitals.
As I recently described on the DocGraph mailing list, work is underway to acquire the data sets that we set out to merge. The issue deals with file formats.
The core identifier for doctors, hospitals and other healthcare entities is the National Provider Identifier (NPI). This is something like a Social Security number for doctors and hospitals. In fact it was created in part so that doctors would not need to use their Social Security numbers or other identifiers in order to participate in healthcare financial transactions (i.e. paid by insurance companies for their services). The NPI is the “one number to rule them” in healthcare and we want to map data from other sources accurately to that ID.
Each state releases none, one or several data files that can be purchased and also contain doctor data. But these file downloads are in “random file format X.” Of course we are not yet done with our full survey of the files and their formats, but I can assure you that they are mostly CSV files and a troubling number of PDF files. It is our job to take these files and merge them against the NPI, in order to provide a cohesive picture for data scientists.
But the data available from each state varies greatly. Sometimes they will have addresses, sometimes not. Sometimes they will have fax numbers, sometimes not, sometimes they will include medical school information, some will not. Sometimes they will simply include the name of the medical school, sometimes they will use a code. Sometimes when they use codes they will make up their own …
I am not complaining here. We knew what we were getting ourselves into when we took on the DocGraph project. The community at large has paid us well to do this work! But now we have a question? What data formats should we support? Read more…
DocGraph: Open social doctor data
An inside look at DocGraph, a data project that shows how the U.S. health care system delivers care.
Notice, October 2015: Certain versions of this data have been retracted. Please read more here.
At Strata RX in October I announced the availability of DocGraph. This is the first project of NotOnly Development, which is a Not Only For Profit Health IT micro-incubator.
The DocGraph dataset shows how doctors, hospitals, laboratories and other health care providers team together to treat Medicare patients. This data details how the health care system in the U.S. delivers care.
You can read about the basics of this data release, and you can read about my motivations for making the release. Most importantly, you can still participate in our efforts to crowdfund improvements to this dataset. We have already far surpassed our original $15,000 goal, but you can still get early and exclusive access to the data for a few more days. Once the crowdfunding has ended, the price will go up substantially.
This article will focus on this data from a technical perspective.
In a few days, the crowdfunding (hosted by Medstartr) will be over, and I will be delivering this social graph to all of the participants. We are offering a ransom license that we are calling “Open Source Eventually,” so participants in the crowdfunding will get exclusive access to the data for a full six months before the license to this dataset automatically converts to a Creative Commons license. The same data is available under a proprietary-friendly license for more money. For all of these “releases,” this article will be the go-to source for technical details about the specific contents of the file.
The Direct Project has teeth, but it needs pseudonymity
How patient pseudonyms can inspire trust in the Direct Project's network.
Yesterday, Meaningful Use Stage 2 was released.
You can read the final rule here and you can read the announcement here.
As we read and parse the 900 or so pages of government-issued goodness, you can expect lots of commentary and discussion. Geek Doctor already has a summary and Motorcycle Guy can be expected to help us all parse the various health IT standards that have been newly blessed. Expect Brian Ahier to also be worth reading over the next couple of days.
I just wanted to highlight one thing about the newly released rules. As suspected, the actual use of the Direct Project will be a requirement. That means certified electronic health record (EHR) systems will have to implement it, and doctors and hospitals will have to exchange data with it. Awesome.
More importantly, this will be the first health IT interoperability standard with teeth. The National Institute of Standards and Technology (NIST) will be setting up an interoperability test server. It will not be enough to say that you support Direct. People will have to prove it. I love it. This has been the problem with Health Level 7 et al for years. No central standard for testing always means an unreliable and weak standard. Make no mistake, this is a critical and important move from the Office of the National Coordinator for Health Information Technology (ONC).
Why microchips in pills matter
Microchips embedded in pills can ease medicine management and empower patients.
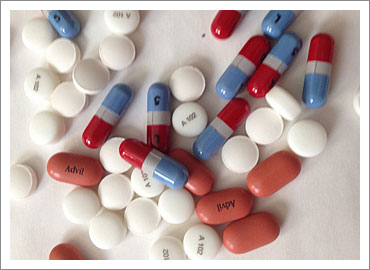 Earlier this week, Proteus announced that they have been approved by the FDA to market their ingestible microchips for pills.
Earlier this week, Proteus announced that they have been approved by the FDA to market their ingestible microchips for pills.
Generally, the FDA approval process for devices that are totally new like this is a painful one, with much suffering. So it is a big deal for anyone to get approved for anything.
But this is a far more important accomplishment than a mere incremental improvement. It is an entirely new kind of medical device and, most importantly, a whole new potential data stream on one of the most critical issues in the delivery of health care.
Modern drugs work wonders, but it does not help a patient if the patient does not take them. Historically, and I do mean the stone age here, the ability to consistently take pills correctly has been called “compliance.” But please do not call it that. Most participants in the movement for patient rights regard that term as paternalistic.
“Adherence” is a much more respectful term (although I have certainly heard it used in a paternalistic manner). In fact, as we progress, I should define that when I say “adherence,” what I mean is “adherence to a plan that belongs to the patient.” If a pill that I am taking makes me so sick to my stomach that I cannot take it any more, then when I decide to stop taking it, I am not being “non-compliant” or “non-adherent” to a medication plan; I have changed my medication plan, and I have yet to discuss the issue with my doctor.
Still, even for patients who want to consistently take their pills according to a plan, it can be extraordinarily difficult. It is hard to remember when a pill has been taken. It is hard to remember to pick up a new supply or to call for a renewal. It is easy to forget pills on trips and run out unexpectedly far from home. Pills frequently must be taken with food, or without food, or with or without specific foods. They must be taken before bed or before breakfast. Personally, I have trouble remembering to take even a single pill consistently. But many people need to manage a tremendous number of pills, and they frequently go off one set of pills and onto another. In short, pill management is a huge mess, and it is difficult to organize anything.
